Abstract
U.S. courts frequently require forensic examiners to offer opinions concerning the likelihood that criminal defendants found incompetent to stand trial can have their competence “restored” through treatment. Yet no jurisdiction has established legal guidelines for testimony concerning restorability, and several authors have suggested that mental health professionals cannot accurately predict whether treatment to restore competence will succeed. This study asked whether reliable information that is consistently available at the time of examination might support empirically grounded opinions about the likelihood of restoration. Using records from all 351 inpatient pretrial defendants who underwent competence restoration at a state psychiatric hospital from 1995 through 1999, I evaluated whether several types of information that are reliable and that could consistently be made available to forensic examiners—including evaluees’ demographic characteristics, diagnoses, symptom patterns, criminal charges, number of prior public sector hospitalizations, and cumulative prior length of stay (LOS)—would predict outcome of restoration efforts. I modeled the probability of successful restoration using logistic regression equations, and evaluated the equations’ predictive accuracy using k-fold cross-validation and receiver operating characteristic (ROC) analysis. Lower probability of restoration was associated with having a misdemeanor charge, longer cumulative LOS, older age, and diagnoses of mental retardation, schizophrenia, and schizoaffective disorder. Although the overall rate of successful restoration for felony defendants was 75 percent, logistic equations allowed selection of subgroups with high predicted probabilities of restoration (>90%) and low probabilities of restoration (<35%). In cross-validation simulations, predictive equations had ROC areas of 0.727 for all defendants, and 0.735 for felony defendants. These findings provide scientific support for testimony that two types of incompetent evaluees have well-below-average probabilities of being restored: chronically psychotic defendants with histories of lengthy inpatient hospitalizations and defendants whose incompetence stems from irremediable cognitive disorders (such as mental retardation). Nonetheless, courts may still deem low probabilities of success to be “substantial” enough to warrant attempts at restoration.
For centuries, Anglo-American legal tradition has barred prosecution of accused criminals who are not mentally fit to defend themselves,1–3 and in the 1960s and 1970s, Supreme Court decisions made assuring the competence of defendants a requirement of U.S. constitutional law.4–6 Under criteria articulated in the landmark decision in Dusky v. U.S., criminal prosecution may not take place unless a defendant “has sufficient present ability to consult with his lawyer with a reasonable degree of rational understanding” and “has a rational as well as factual understanding of the proceedings against him” (Ref. 4, p 402).
All U.S. jurisdictions have procedures for holding hearings and making determinations about a criminal defendant's adjudicative competence, or (to use the more common term) competence to stand trial (CST). Recent estimates suggest that each year 50,000 to 60,000 U.S. defendants undergo examinations to determine CST.7,8 In about one fifth of these cases, trial courts conclude that defendants are incompetent.9,10 Once they are found incompetent to stand trial (IST), most defendants undergo court-ordered “restoration”—mental health treatment and/or education aimed at enabling defendants to proceed with adjudication.11,12 On any given date, defendants hospitalized for competence restoration occupy roughly 4,000 psychiatric hospital beds in the United States, or about one ninth of the nation's state psychiatric hospital beds.13–15
Inpatient restoration cannot be the automatic result of a trial court's finding of incompetence, however. In Jackson v. Indiana,16 the U.S. Supreme Court held that it violated a pretrial defendant's constitutional right to due process to subject him to indefinite hospitalization solely because he was incompetent to stand trial. Under Jackson, an incompetent criminal defendant may not “be held more than the reasonable period of time necessary to determine whether there is a substantial probability that he will attain that competency in the foreseeable future” (Ref. 16, p 738).
Most U.S. jurisdictions require examiners who believe that a defendant is IST to offer an opinion concerning the likelihood of the defendant's regaining competence if provided with a course of treatment.17,18 Yet no jurisdiction has established legal guidelines concerning testimony about potential restoration, and previous publications suggest that mental health professionals encounter problems in making predictions about restorability.
A few years after the Supreme Court issued Jackson, Roesch and Golding19 asserted that mental health professionals could not accurately assess the likelihoods of defendants’ becoming competent with treatment, in part because the high base rate of successful restoration made it difficult to detect defendants who would not respond to treatment. Indeed, studies of defendants from Los Angeles,20 Michigan,21 Ohio,22,23 and Oklahoma,24 have shown that most defendants hospitalized for competence restoration regain their competence, and the few studies that examine prediction accuracy have yielded results that tend to confirm Roesch and Golding's pessimistic assessment.
An Illinois study found that clinicians were wrong in predicting treatment outcomes of 85 percent of the defendants who ultimately were not restored,25 and Florida researchers concluded that a discriminant function they developed had “little or no better than chance utility in predicting” restorability (Ref. 26, p 73). A retrospective Oklahoma study17 found that having a previous criminal record and alcohol use at the time of the offense modestly increased the likelihood of competence restoration; impairment in psycholegal ability, having psychotic symptoms, and aggression toward others after arrest were correlated with failure to attain competence. Nonetheless, the study's authors concluded that their results were “consistent with prior research in suggesting that examiners should exercise caution in providing feedback to courts concerning [the likely success of] competency restoration” (Ref. 17, p 377). A recent Alabama study18 found few differences between defendants who examiners predicted were restorable or nonrestorable. Those differences that did exist reflected mainly nonpsychiatric variables such as criminal record, current criminal charge, and understanding of the legal process.
Summarizing previous research findings in the mid-1990s, Nicholson and colleagues concluded “that the ability of clinicians to predict competency restoration is poor, at least when compared with the base rate of failed restoration” (Ref. 17, p 373). Yet this conclusion seems at odds with research that has demonstrated associations between patient characteristics and treatment outcomes. For example, “[a] plethora of studies” (summarized in Ref. 27, p 48) have linked patients’ clinical, demographic, and biological characteristics to good antipsychotic drug response. In addition, research suggests that certain patient characteristics, including duration of illness and lifetime hospitalization, are associated with lack of improvement during antipsychotic therapy.28 It therefore seems reasonable to suppose that certain types of clinical information would provide a scientific, empirically grounded basis for forensic examiners’ opinions about potential restorability. In the present study, I attempted to find out whether the types of reliable information that could be made consistently available when competence examinations take place might provide an empirical basis for forensic opinions about the likelihood of restoration.
Methods
Setting
This study used archival data from 1995 through 1999 admissions to a public-sector psychiatric hospital in Ohio. During the study period, the hospital served patients from four metropolitan areas and several suburban and rural regions. At the hospital, inpatient pretrial defendants undergoing competence restoration received several types of clinical interventions as deemed appropriate by their hospital clinicians. Most competence restorees participated in group psychotherapies (along with patients hospitalized for other reasons) designed to help patients understand their medication, develop better interpersonal skills, and refrain from drug misuse. Most IST patients with psychoses received either conventional or atypical antipsychotic drugs; those patients thought to have affective syndromes usually received mood stabilizers or antidepressants. Competence restorees participated in group didactic sessions focused on improving their factual grasp of legal proceedings, legal pleas, potential trial outcomes and consequences, and the roles of courtroom personnel. IST patients often received additional individual instruction aimed at helping them to understand and make decisions concerning their own legal cases.
Treatment teams (including a psychiatrist, a psychologist, a social worker, and a nurse) assessed patients’ progress toward competence at least monthly. Patients regarded as competent by their treatment teams usually were discharged from the hospital to jail, to await disposition of their criminal cases.
Statutory Schemes
IST patients came to the hospital under two statutory schemes. Before July 1997, criminal courts in Ohio could order hospitalization only for incompetent defendants found to have a “substantial probability” of becoming competent with treatment. In felony cases, restoration efforts could last no longer than one third of the defendant's minimum sentence if convicted, up to a maximum of 15 months. Defendants charged with misdemeanors could receive treatment for up to one third of their maximum potential sentence, which translated into treatment periods of 10 to 60 days. In the last half of the study period, Ohio law required criminal courts to order treatment for all incompetent defendants. Depending on the seriousness of their charges, maximum restoration periods were 4 to 12 months for felony defendants and 30 to 60 days for misdemeanor defendants. (After the study period, the Ohio Supreme Court ruled the latter statutory scheme unconstitutional because it required treatment even when efforts at restoration would be futile.29)
Under both statutory schemes, defendants who did not achieve competence during the statutorily permitted period had their charges dismissed. They then became subject to possible civil commitment and could face reindictment if released from the hospital before the statute of limitations had expired.
Procedures
This study received approval from the Institutional Review Board of Wright State University and from the Ohio Department of Mental Health (ODMH). Using computer and file records, I identified 351 treatment episodes that began in the years 1995 through 1999 in which IST patients underwent competence restoration. This five-year period was chosen because it was fairly recent, because referrals to the hospital and treatment of IST patients had been relatively homogeneous over the time span, and because all IST patients admitted during this five-year span had completed efforts at competence restoration when data collection began in late 2001.
An unanticipated feature of the 1995 through 1999 study period stemmed from the jurisdiction's practices concerning forced medication for refusing patients. Under these practices (which changed after the June 2003 Sell v. U.S. decision30), defendants usually came to the hospital with court orders that authorized administration of psychotropic medication irrespective of the defendants’ wishes. When this had not occurred, trial courts would promptly issue orders authorizing involuntary medication after receiving notice from the hospital that a patient was refusing treatment. Once patients began receiving medication, clinical staff members employed various means to make sure patients were receiving and not diverting prescribed medications (e.g., administering liquid forms of medication, checking patients’ mouths after administration, or having patients remain where they could be observed so that they would not surreptitiously regurgitate the medication). Whatever one thinks about the wisdom or constitutionality of these practices, they meant that this study could evaluate predictors of restorability (including medication responsiveness) of all IST defendants referred to the hospital.
Figure 1 describes the selection of files for data analysis. Excluded from analysis were the records of two patients who did not complete attempts at restoration at the hospital (one patient was transferred to another hospital after a few days; one patient died a few days after admission). In another 21 cases, hospitalizations represented patients’ second or third episodes of competence restoration during the study period. To avoid statistical problems that might arise from multiple observations of the same subjects, I limited analyses to these patients’ first episode of competence restoration. The remaining 328 episodes of care represented attempts at restoration for 268 felony defendants and 60 misdemeanor defendants. Table 1 provides detailed information about the patients’ characteristics.
Selection of files for data analysis, showing the number of patients charged with felonies and misdemeanors and outcomes of restoration efforts.
Characteristics of 328 Patients Undergoing Competence Restoration and Performance of Each Characteristic as a Predictorof Restoration
Computer databases provided patients’ demographic information (sex, ethnicity, marital status, admission date, and birth date), multiaxial admission diagnoses, number of previous ODMH (i.e., public sector) hospitalizations, and cumulative length of stay (LOS) for all previous ODMH hospitalizations. The treating psychiatrists had rendered these diagnoses based on their patients’ clinical presentations and all available psychiatric history, applying then-current DSM-IV criteria. Hospital charts (which contained photocopies of court filings) provided information about patients’ criminal charges.
Before beginning treatment, each IST patient had undergone at least one court-ordered CST evaluation, usually performed by a local forensic assessment center independent of the hospital. Most referring courts provided the hospital with the written reports from these evaluations. For this study, I reviewed these reports and abstracted any information about specific symptoms that the competence examiners had adduced as directly responsible for each patient's incompetence. When copies of court-ordered reports were not on file, I reviewed the patient's admission psychiatric examinations for information about symptoms responsible for his adjudicative incompetence. Each incompetence-causing symptom was then classified as belonging within one of the four main components or symptom clusters—manic excitement/disorganization, depression/anxiety, negative symptoms, and positive symptoms—of the expanded Brief Psychiatric Rating Scale (BPRS–E), as described by Ruggeri and colleagues.31 If more incompetence-causing symptoms fell within a single cluster than in any other single cluster, that cluster was recorded for the patient. (For example, suppose a report indicated four incompetence-causing symptoms for a patient. If two were positive symptoms, one was a negative symptom, and one was a depression/anxiety symptom, then “positive symptoms” was recorded for that patient.) Subsequently, this characterization of incompetence-causing symptoms was evaluated as a possible predictor of restorability.
Rationale for Variable Selection
Table 1 lists the study variables. Predictors to these variables were restricted for two reasons. First, the limited size of the database suggested that evaluating many more potential predictors might produce spuriously “significant” correlations. (Because predictors might be correlated but the degree of correlation was unknown, I could not use any simple Bonferroni-type level-of-significance correction to offset the statistical impact of multiple comparisons in the same variable set.) Second, I wished to evaluate only variables that had plausible potential relationships to restorability and that reflected information that evaluators could—and did—ascertain reliably at the time of evaluation or hospital admission.
Other patient characteristics (e.g., years of education, highest Global Assessment of Functioning Scale score for the past year, duration of illness, cumulative duration of treatment at non-ODMH facilities, and past responses to treatment) might have been useful indicators of restorability. Experience had shown, however, that evaluators often did not carefully explore these matters or could not obtain accurate information about them at the time of evaluation; thus, these factors could not function as reliably scored predictor variables. By contrast, demographic data, ODMH hospitalization history, currently observed symptoms, and initial diagnostic impressions were ascertained and recorded consistently. Including the number and cumulative duration of patients’ previous public sector hospitalizations provided reliable (though imperfect) proxy indicators of effectiveness of patients’ previous treatment and the chronicity of their illnesses.
Admission dates were examined as a possible predictor to find out whether the mid-1997 statutory change affected the likelihood of success at restoration. I evaluated the presence or absence of retardation as a possible predictor variable, but not the severity of retardation, because all but three of the patients with diagnosed mental retardation were deemed to have “mild” retardation.
Outcome Criterion
My criterion for restoration was the treatment team's final assessment of each patient's competence. Three reasons supported using treatment teams’ judgments rather than the ultimate determinations by referring trial courts. First, in most cases, criminal courts accepted hospital clinicians’ opinions without hearing testimony or conducting any independent investigation of a defendant's competence. Second, I wanted to use a competence criterion that was uniform across patients, and I believed that opinions of clinicians at a single treating institution would be more uniform than opinions of dozens of criminal courts. Third, most instances in which trial courts’ findings differed from the hospital's opinions involved former patients whom clinicians had treated and (in their opinion) restored to competence, who had returned to jail to await disposition, and who then experienced relapses or deterioration (frequently because the former patients stopped receiving medication after leaving the hospital). Given such instances, it seemed reasonable to assume that clinicians had made accurate assessments before hospital discharge and that courts’ later findings of incompetence reflected post-hospitalization changes in defendants’ mental conditions.
Statistical Procedures
Exploratory analyses individually examined each variable's capacity to predict success at restoration. Because misdemeanor defendants had statutorily truncated periods to regain competence, I evaluated variables using results for all 328 IST patients and for the 268 felony defendants alone. Backward stepwise logistic regression (implemented with SPSS 10.0 software using the likelihood ratio test) was used to generate prediction equations for all 328 IST patients and the 268-member subgroup who faced felony charges. When generating prediction equations, I coded as +1 or 0 the presence or absence of schizophrenia/schizoaffective disorder, mental retardation, felony charge, African-American ethnicity, diagnosis of substance use. The patients’ ages, their numbers of prior ODMH hospitalizations, and their previous ODMH hospitalization days were entered as numeric values. The removal criterion was set at .01 to minimize “overfitting” of the prediction equations, but the reentry criterion was set at .05.
If one uses the same set of subjects both to produce a prediction procedure and to evaluate its accuracy, any resulting accuracy statistics will probably be overoptimistic (i.e., will overestimate the procedure's true accuracy in future subjects). Therefore, the accuracy of the prediction equations was assessed with k-fold cross-validation (with k = 10), a procedure that produces a nearly unbiased estimate of prediction accuracy.32 The accuracy of the cross-validation “predictions” was quantified by using receiver operating characteristic (ROC) methods.
Results
Demographic and diagnostic variables of the patients appear in Table 1, accompanied by test statistics concerning each variable's association with competence restoration. For the full cohort of 328 IST patients, eight variables—misdemeanor charge, age at admission, mental retardation, having schizophrenia or schizoaffective disorder, number of previous ODMH hospitalizations, and cumulative previous LOS at ODMH hospitals, non-African-American ethnicity, and having a substance use disorder—were individually associated at the p < .05 level with reduced likelihood of restoration. Among the felony defendants, however, ethnicity and substance use diagnoses were not significantly associated with failure of restoration efforts. Stepwise logistic regression yielded the following three-variable predictive equation for the probability p of competence restoration among the full 328-member cohort of competence restorees: 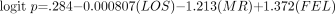 (1) In Equation 1, “logit p” equals the natural (Naperian) logarithm of p/(1 − p), LOS denotes the patient's previous cumulative LOS, MR equals +1 if the patient had mental retardation and 0 otherwise, and FEL equals +1 if the patient faced a felony charge and 0 for a misdemeanor charge. The k-fold cross-validated value of the area under the curve (AUC) for Equation 1 was 0.727 ± 0.028 (p < 10−5), equivalent to an effect size of d = 0.853.
(1) In Equation 1, “logit p” equals the natural (Naperian) logarithm of p/(1 − p), LOS denotes the patient's previous cumulative LOS, MR equals +1 if the patient had mental retardation and 0 otherwise, and FEL equals +1 if the patient faced a felony charge and 0 for a misdemeanor charge. The k-fold cross-validated value of the area under the curve (AUC) for Equation 1 was 0.727 ± 0.028 (p < 10−5), equivalent to an effect size of d = 0.853.
Equation 1 implies that facing only a misdemeanor charge substantially reduced the odds of regaining competence. Given the relatively brief restoration periods permitted misdemeanor defendants, this finding was expected. Including misdemeanor defendants in the analysis may, on the one hand, have artificially improved classification accuracy by including a marker for patients who had relatively short treatment episodes. On the other hand, including misdemeanor defendants may have statistically obscured other predictors of successful restoration when patients have longer treatment periods. I therefore evaluated potential predictors among the 268-member subgroup of felony defendants and obtained this equation: 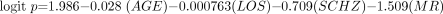 (2) In Equation 2, logit p, LOS, and MR have the same meanings and codings as in Equation 1; AGE is the patient's age when admitted; SCHZ was coded +1 if the patient's diagnosis was schizophrenia or schizoaffective disorder, and 0 otherwise. The AUC for this k-fold cross-validated predictive equation was 0.735 ± 0.032 (p < 10–5), equivalent to an effect size of 0.889.
(2) In Equation 2, logit p, LOS, and MR have the same meanings and codings as in Equation 1; AGE is the patient's age when admitted; SCHZ was coded +1 if the patient's diagnosis was schizophrenia or schizoaffective disorder, and 0 otherwise. The AUC for this k-fold cross-validated predictive equation was 0.735 ± 0.032 (p < 10–5), equivalent to an effect size of 0.889.
The AUC and effect size associated with Equation 2 imply that it does a respectable job of sorting restorable and nonrestorable defendants. But another way to evaluate the usefulness of a predictive equation is to consider whether it would let an evaluator identify a subgroup of IST defendants with probabilities of successful restoration that are well above or well below average. Setting p in Equation 2 at <.35 identified 18 IST felony defendants whose cross-validated probabilities of restoration were 35 percent or lower; of these 18 patients, only 5 (28%) achieved competence. For these patients, the median and average cumulative total LOSs were more than 10 years before they began efforts at competence restoration; their average age was 40.1 years; 14 (78%) of them had schizophrenia or schizoaffective disorder; and 8 (44%) had mental retardation.
By contrast, of the 60 patients facing felony charges who had the highest cross-validated probabilities of becoming competent, 56 (93%) were in fact restored. These 60 patients averaged just 24 days of total prior hospitalization; their average age was 26.6 years, only 7 (12%) of them had schizophrenia or schizoaffective disorder, and none had admission diagnoses of mental retardation. It is interesting to note that among the four nonrestored patients in this highest probability group, two had admission diagnoses of psychotic disorder not otherwise specified but discharge diagnoses of schizophrenia or schizoaffective disorder; the third patient had mental retardation diagnosed later in the hospitalization; and the fourth had a cognitive disorder attributed to congenital “brain damage.” Thus, all four unrestored defendants from the 60 patients with the highest probabilities turned out to have conditions that this study suggests would reduce the likelihood of restoration.
Discussion
Most U.S. jurisdictions require examiners who conclude that a defendant is IST to offer an opinion concerning the likelihood of the defendant's regaining competence after treatment. In contrast to findings in several previous publications, this study suggests that specific clinical data could help competence examiners assess restorability.
Reasons for Success
The success of this study may have resulted from the use of variables that have plausibly strong relationships to being educable and likely to respond to treatment. I was especially fortunate to have data that identified patients who had spent many years of life hospitalized in public sector facilities, a clinical indicator implying poor response to past treatment efforts and probable poor response to future efforts. Individuals with mental retardation have (by definition) well-below-average intellectual ability, which a fortiori limits their capacity to grasp issues related to criminal proceedings. The correlation between age and restoration failure is consistent with studies indicating better antipsychotic response in younger individuals.33–37 The comparative difficulty of restoring individuals with schizophrenia or schizoaffective disorder may reflect the neurocognitive deficits that underlie these conditions.38–40
I also may have had more success than previous investigators because of my jurisdiction's statutes and my method of selecting subjects. I examined records of all defendant-patients referred to my facility after they had completed statutorily defined restoration periods that were limited to 15 months. In contrast, previous investigators examined populations after just three months of hospitalization,26 restricted their study population to discharged patients who came from a jurisdiction with an unspecified period for competence restoration,24 or studied patients where the statutorily permitted restoration period was much longer.17 Assessing patients after just three months of treatment may lead one to misclassify some not-yet-competent-but-ultimately-restorable patients as simply unrestorable, and this may impede identification or optimal statistical weighting of variables that would predict ultimate outcome. Restricting the study group to discharged patients excludes the most impaired defendants, which may bias apparent outcomes and the value of possible predictor variables.24 In jurisdictions with lengthy (unspecified or multiyear) restoration periods, some individuals who are treatment-resistant may become CST simply because of random variation in the severity of their illness rather than because they have received specific treatments. Including such patients might statistically obscure the value of variables that predict response to therapy.
Implications
Because this study's data came from a single state, a single facility, and a limited time period, I do not recommend that forensic examiners use my predictive equations to calculate probabilities of restoration. Rather, my findings provide support for two circumstances in which mental health experts may opine that treatment will have a low chance of restoring a felony defendant's adjudicative competence. First, if a defendant is incompetent because of a longstanding psychotic disorder that has resulted in lengthy periods of psychiatric hospitalization, this history supports an opinion that the defendant has a well-below-average probability of becoming competent with psychiatric treatment. Second, if a defendant has an irremediable cognitive disorder (e.g., mental retardation) and can grasp little information that the examiner attempts to convey during an evaluation, this finding would support a conclusion that restoration efforts will have well-below-average chances of success.
Though the previous paragraph's conclusions seem obvious, this is the first study to provide empirical support for them. Moreover, these findings provide a counterweight to previous conclusions that evaluators’ ability to predict restoration is “poor” or “no better than chance.” My findings suggest that, before rendering opinions about restorability of apparently incompetent defendants, forensic examiners may want to explore more carefully whether cognitively limited defendants have mental retardation and may want to review more carefully the collateral information about chronically psychotic defendants’ treatment and hospitalization histories. Readers should note, however, that even when an evaluator identifies a defendant with a well-below-average probability of restoration, that defendant's likelihood of becoming competent with treatment may still be “substantial” enough for a court to order time-limited attempts at restoration. As the present study shows, even among defendants who had the lowest predicted probabilities of regaining competence, more than one-fourth became competent after treatment.
Limitations
My findings are limited by the retrospective, uncontrolled nature of this study. Also, I relied on archival data in hospital records, which contained conscientiously assembled but unsystematic observations and conclusions about patients. For this study's purposes, it would have been desirable to have forensic examiners systematically document defendants’ symptoms using structured instruments, to have treating clinicians use structured interviews when arriving at diagnoses, and to have degrees of improvement in competence quantified by using standardized assessment instruments.
Yet these and other limitations in the study prompt five comments in defense of my efforts:
First, although some forensic patients may welcome the chance to participate in research,41 CST evaluees often will not or cannot participate in detailed, systematic assessments. I used data that always are or could be available for every evaluee.
Second, when most of the subjects underwent evaluation and restoration, then-available instruments for assessing competence focused mainly on defendants’ factual knowledge, and did not measure defendants’ appreciation of or ability to reason about their situation.9 Moreover, even the best currently available assessment tools are not meant to supplant clinicians’ judgments, but to function only as guides for evaluators.42,43
Third, prospective studies using systematic assessment measures have the drawback of not including individuals who will not or cannot give consent to participate. In the case of competence restorees, this could be a substantial fraction of potential subjects.44 After all, IST defendants are, by definition, impaired in their capacity to grasp information and/or collaborate. By contrast, this study, though limited to archival data, included every patient who underwent competence restoration at my facility during the study period.
Fourth, IST patients are usually hospitalized under court order and frequently face serious charges. For these patients, the outcome of “successful” treatment is often prosecution and punishment.15 Any prospective study that alters what otherwise would take place during a defendant's evaluation or treatment could affect the course of an ongoing criminal case. By using typical (if flawed) information available from already completed treatment episodes, this retrospective study obviated potential ethics concerns about changing the outcome of a defendant-patient's treatment or prosecution.
Finally (and notwithstanding the previous point), I have identified factors that could be evaluated systematically and prospectively by other investigators working in different jurisdictions and with larger subject populations, without intruding inappropriately on legal proceedings or the ordinary process of assessment. For example, it would not be difficult for forensic evaluators to complete a BPRS for each evaluee using data ordinarily available from interviews, nor would it pose a problem for evaluators to complete a checklist indicating the principal signs or symptoms of illness that they believe are the causes of an incompetent evaluee's inability to stand trial. Although incompetence-causing symptom clusters were not predictive of restoration in this study, a more systematic assessment of symptoms during evaluation might yield a different finding. It also might be useful to study whether, at the time of evaluation, examiners could actually get better information about diagnoses, effectiveness of past treatment, or other indicators of illness chronicity and whether having such information would improve prospective assessments of restorability.
Conclusions
In contrast to previous reports, this study provides reason for some optimism about developing empirical guidelines for expert opinions about competence restoration. I hope the reported results will encourage other investigators to study a topic that affects many criminal defendants and a large fraction of patients in public-sector hospitals.
Acknowledgments
Thanks to Douglas S. Lehrer, MD, for assistance with study conceptualization and design, to the late Ann Murray, MD, for assistance with data gathering, and to the anonymous reviewers for their advice concerning an earlier version of the article.
- American Academy of Psychiatry and the Law












